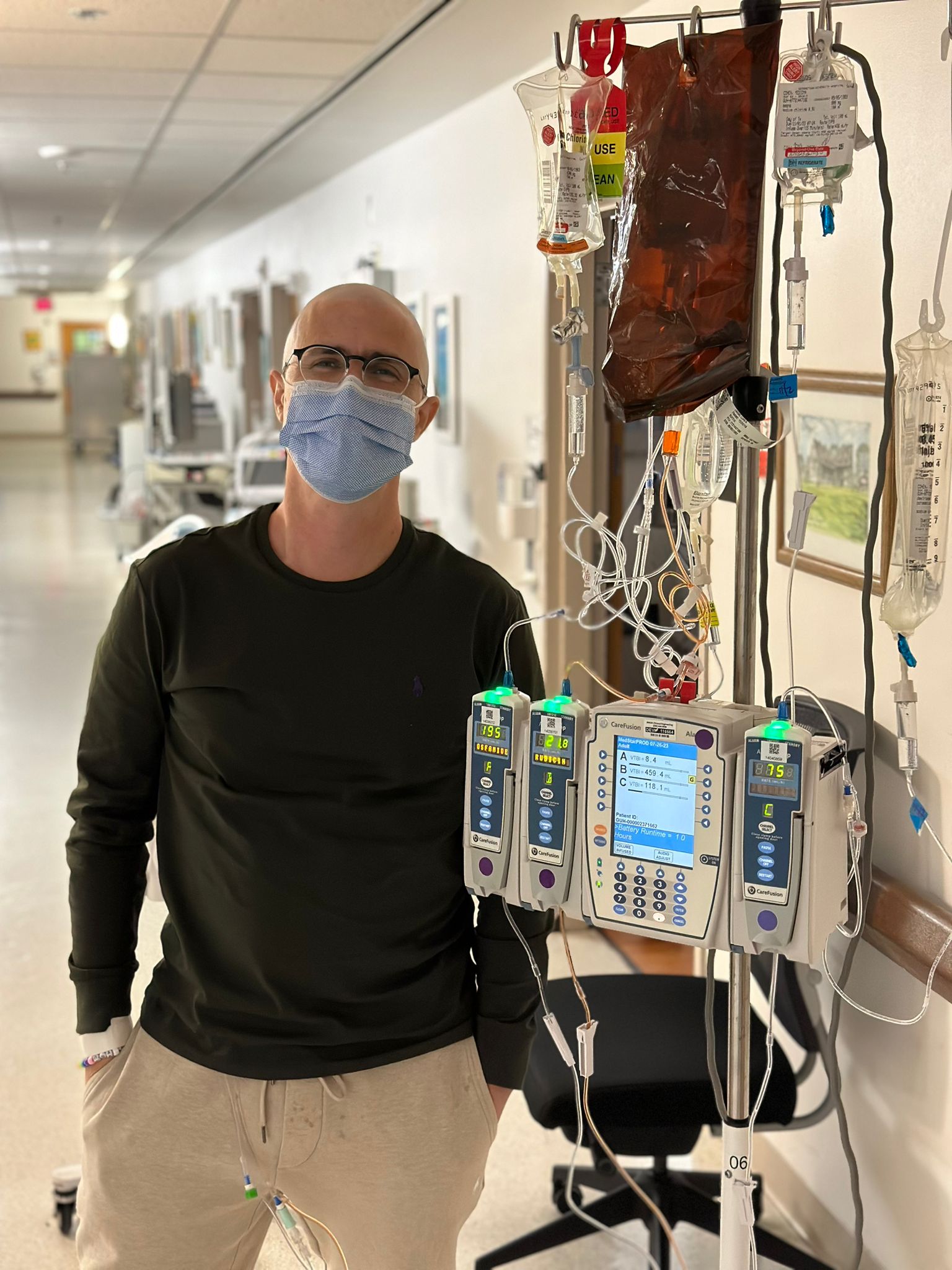
"Receiving a synovial sarcoma diagnosis can be scary and overwhelming. It certainly was for me. My initial response was panic and fear. I had so many questions."
- Eddie Cohen
I’ve realized that there isn’t much information online about the synovial sarcoma patient experience. When I was diagnosed in 2023, I struggled to find information from a patient perspective about diagnosis, treatment, recurrence, and beyond.
In the posts that follow, I will share my experience and critical information I learned through my cancer treatment journey. My hope is to play a small part in minimizing a critical information Gap.
If there is a topic I have not covered or that you would like me to cover in greater depth, please comment or send me a direct message.
Synovial sarcoma is a rare and aggressive soft tissue cancer that accounts for 5-10% of soft tissue cancers and often affects younger individuals.
It’s called “synovial” sarcoma because its cells resemble cells in synovial joints such as such as shoulders and elbows.
Synovial sarcoma often appears first in the knee, ankle, arm, wrist, or hand. However, it can develop in a variety of other locations such as the head, neck, lungs, or abdomen.
Although we are still learning about the cause of synovial sarcoma, we know that it relates to a gene mutation / translocation.
Tumors in the soft tissue can often be seen on an MRI and tumors in the lung can often be seen on a CT scan or X-ray. However, a diagnosis requires review by a pathologist of tissue obtained through biopsy or surgery.
Although some patients identify that something is wrong when they find a lump or experience pain, others (like me) may be completely unaware that a tumor is developing inside their body.
September 1, 2023. I arrived in Rio De Janeiro with my husband, @Nathan Imperiale, to celebrate a milestone birthday. I always dreamed of visiting Brazil and we were finally there…
September 2, 2023. I woke up to the worst pain I had ever felt in my life. Barely two steps out of bed, I stumbled and fell to the ground, unconscious. I thought I was dying. Thanks to my husband's quick thinking, I was rushed to CopaStar Hospital.
Doctors initially suspected kidney stones but, out of an abundance of caution, ordered a chest CT. To everyone’s surprise, they found a large mass surrounded by blood and fluid in my left chest cavity.
The week that followed was frightening. Was this cancer or a benign tumor? How was I going to get home? I am forever indebted to the doctors and staff at CopaStar – including mention specific doctors - for stabilizing me so that I could travel back to the United States.
It would take another month before I received a definitive diagnosis of synovial sarcoma. In the meantime, I spent 10 nights in the hospital with chest tubes installed to drain the fluid from my chest. The first five nights were spent in isolation because, unbeknownst to me, I also had (latent) tuberculosis.
Receiving a synovial sarcoma diagnosis can be scary and overwhelming. It certainly was for me. My initial response was panic and fear. I had so many questions. “What is synovial sarcoma and how do we treat it?” “What comes next?” “How long am I going to live?”
Not all synovial sarcoma is created equal.
Tumors can be differentiated based upon the HLA proteins that are found on the surface of their cells. Thus, there are different “HLA subtypes” of synovial sarcoma. Additionally, some
tumors express certain proteins/antigens – such as NY-ESO-1 or MAGE-A4 - that others do not.
Why is early biomarker testing important?
Biomarker testing is used to identify your HLA subtype and whether your tumor expresses specific proteins. Since specific treatments or clinical trials may only be available to patients with a certain HLA-type, or whose tumor expresses certain proteins, early biomarker testing is Critical.
For example, in order to receive TECELRA, the first FDA-approved T-cell therapy for synovial sarcoma, you must have one of the following HLA types: HLA-A*02:01P, HLA-A*02:02P, HLA- A*02:03P, or HLA-A*02:06P (and must not have HLA-A*02:05P), and whose tumor expresses MAGE-A4.
I was not eligible for Tecelra based upon my HLA type but I do qualify for Letecel, another revolutionary T-cell therapy for synovial sarcoma that is currently going through the approval Process.
How do I get biomarker testing?
Biomarker testing is availability through national and specialty labs, including Caris, Life Sciences, and Tempus. More information and printable guides to share with your care team are available at www.sarcomabiomarkertesting.com.
Although biomarker testing is expensive, financial resources may be available to you. For example, if you believe Tecelra may be a treatment option and you need help accessing testing or therapy, visit www.tecelra.com/adaptimmuneassist.
Sarcoma accounts for only 1% of adult cancers and synovial sarcoma accounts for only 5-10% of sarcomas. That means that many oncologists have never treated a patient with synovial sarcoma and few have treated many of them.
Given the consequences of the advice being given, and the complexity involving in treating synovial sarcoma, I urge fellow patients to: (1) seek care at one of the nation’s many sarcoma centers of excellence; and (2) get a second opinion.
Resources are available, including funding for second opinions from organizations such as the Sarcoma Alliance.
As a lawyer, I am an experienced advocate. However, learning to navigate hospital systems, and effectively advocate for my own care, is a unique skill that I had little prior experience with.
- Relationships Matter: become somebody that your medical team WANTS to help by being courteous, kind, and reasonable.
- Balance persistence and patience: doctors and hospital staff are extremely busy. Advocate for your needs and follow up while also recognizing that you are one of many patients that your medical team is treating.
- Learn to use the portal: many medical providers in larger hospital systems communicate only through an online portal. The portal can be your friend. Learn how to use it.
- Bring a family member or friend: it can be incredibly valuable to have a family member of friend who can regularly accompany you at appointments, take notes, and help make sure you ask the important questions and follow through with next steps.
Eddie's Synovial Sarcoma Timeline
We are committed to being a business that balances purpose with profit that create value for all our stakeholders.
Eddie traveled to Brazil to celebrate his 40th birthday. On the first morning, he experienced severe pain and was taken to the hospital, where doctors identified a large mass in his chest.
September 2023
After returning to the United States, additional testing confirmed synovial sarcoma. He began meeting with his care team to plan next steps.
October 2023
Eddie started chemotherapy soon after diagnosis. The treatment involved multiple inpatient hospital stays and was physically demanding, requiring close monitoring throughout each cycle.
Fall–Winter 2023
He underwent surgery at the University of Pennsylvania to remove the tumor. The surgery was successful, with clear margins achieved, and part of his lung was preserved. He was declared NED (No Evidence of Disease).
December 2023
Following treatment, Eddie focused on recovery and gradually returning to daily life. He continued regular scans and follow-up care while settling back into his routine.
2024
A routine scan showed a recurrence. Eddie underwent a second surgery, which was successfully completed and he was declared NED again.
February 2025
Eddie continues with regular monitoring and follow-up care. He is actively engaged with the Synovial Sarcoma Foundation, supporting research and advocating for greater awareness and collaboration within the community.